Type 2 diabetes is now one of the world’s most common long term health conditions. Currently, the number of people diagnosed with diabetes in the UK is estimated to be 3.5 million, but taking into account the number of people likely to be living undiagnosed, the real number is over 4 million. This represents 6% of the UK population or 1 in every 16 people having diabetes (diagnosed and undiagnosed). Diabetes prevalence in the UK is estimated to rise to 5 million by 2025.
The disease is described by the medical profession as a progressive, lifelong condition, but as people around the world are proving this very well might not be the case. One man who proved that these symptoms can be reversed is Richard Shaw. After being diagnosed with type 2 diabetes in 2012 he was left with the prospect of an uncertain, pill filled future, until that is, inspired by results obtained from research done at Newcastle University, UK, he decided to try and beat the disease by following a carefully structured, low-carb, whole-food diet and starting an exercise regime.
His book Conquer Type 2 Diabetes details the road he took back to wellness along with the techniques and recipes he created to do so. We spoke to him about his inspirational story that serves as a beacon to the 400 million-plus sufferers worldwide that with a bit of hard work and discipline type 2 diabetes can be put into remission.
The MALESTROM: Can we start by talking about your journey?
Richard Shaw: So I woke up one day and couldn’t see properly, that was the first hint that something was wrong. I had this slightly weird side effect, this thing where the lens suddenly changes its refractive qualities. I was abroad at the time, so I flew home and went to see my optician to tell him there’s something terribly wrong with my prescription.
He told me to go to the hospital as he thought it was something more. So I went there and they tested me and wondered aloud how high my sugar levels had been 24-hours earlier and I walked out with a pile of pills. Then I went to see my GP the following week and she read me my scores and outlined the issue and how we were going to deal with it.
I’d been experiencing the classic signs of diabetes for some weeks leading up to it and not knowing. I’m sure a lot of people are wandering around with pre or full diabetes.
TM: What are those symptoms?
RS: There are three classic symptoms. One is drinking a lot because you’re incredibly thirsty. One is peeing a lot and the other bizarrely is slightly unexpected weight loss. And these are the classic symptoms for having type 2.
Men have a higher propensity to get the disease rather than women, 25% more chance. I think we are less inclined to do anything about our health, we ignore things when they come up.
TM: So how did you find a route to recovery?
RS: I didn’t know anything much about diabetes for three years because everyone told me that I’d be on pills for life. It wasn’t until I read the research coming out of Newcastle by a guy called Roy Taylor, who’s just extraordinary, who proved, at least to my mind, that if you intervene dramatically enough with a significant amount of weight loss then there’s a chance of going into remission.
Now I couldn’t do what he did for the purposes of research to prove his case, which was an ultra-low calorie diet, he puts his subjects on maybe 600-800 calories per day, but he’s doing that for a particular purpose. So I thought I’m going to have a go at doing this my own way and came across quite a big low-carb movement, which was not news to everybody else. So I became an evangelist for it, did it for five months, lost a whole bunch of weight, without really my doctor being a part of it.
I think GPs are a little bit suspicious of this kind of stuff. Anyway, I walked back into her surgery and she looked at me and was like “what the hell“. She took some tests and said “well, I’ve never really seen this before“. She didn’t really quite know what to do with the tablets, like the Metformin, so a few weeks later I just stopped taking the pills and then six months later I went in for more tests and it had worked.
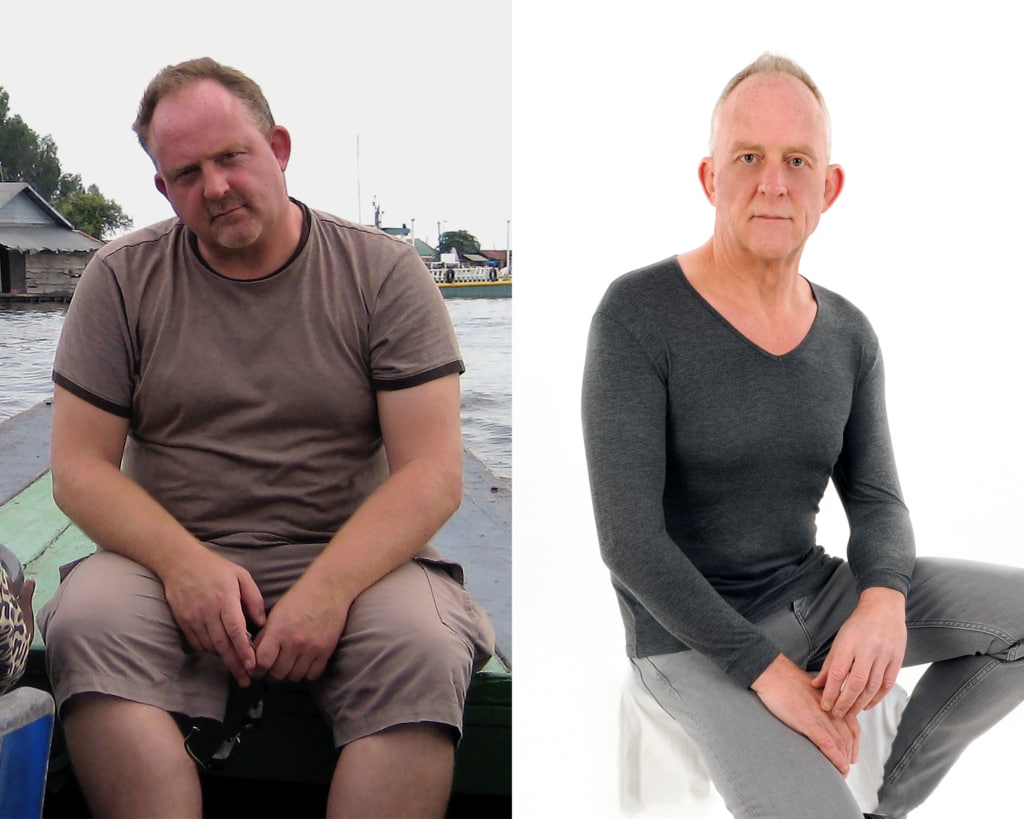
I kept a diary as I was doing it and that turned into my book. So I went from a big guy to a thinner guy and I think the thing that turned my mind was that emerging science from Newcastle which made me think it might be possible as there were a large number of cases where this was put into remission when I had previously been told this is it, this is forever.
TM: It seems doctors are quite hardline on the condition being non-reversible, you and other people have proved this isn’t quite the case, you’d hope the medical profession would follow suit in that thinking?
RS: I think it’s quite a slow process to change public health advice and medical training, some doctors maybe trained 30 years ago and phrases like lifelong condition and progressive are burned into their vocabulary. I think that the way the public health system treats a diabetic is through a process of numbers. You get prescribed pills, you get given a fairly lame piece of lifestyle advice and then your in the system.
Because there are so many people with the condition it’s tricky to come up with an individualised management program to persuade people to try and do enough work to help them get into remission. So I think it’s a challenge. There are also issues around dietary advice that are just terrible. To do something about it it’s going to take a different intervention to make a dramatic social change.
TM: Do you feel that advice given by doctors and nurses needs a serious update?
RS: I think it comes on several fronts. One is a lot of people have this now, so time is short. Your local diabetes clinic is focussed on treating the underlying symptoms, not the cause. So it’s about eye exams, foot health, waist measurement, slightly lame lifestyle advice, be fitter, eat better and so on along with a leaflet, but you have to be out in 25 minutes.
So that’s one issue, time is short in the local diabetes deck. The second issue is there are generational problems around the public health advice. I aimed my particular fury at the guide which has around a third of its dietary recommendations around starchy carbohydrates, which for somebody who’s trying to lose a dramatically large amount of weight is not the way to go.
I just don’t think it’s right. If you want to do something about type 2 you need to get rid of carbs and refined sugars all together for a period of time.
TM: What did a typical meal look like for you pre-diabetes?
RS: I was a comfort food eater, I had a lifetime in food, making TV food programmes, training as a chef. I made bread, and risottos and my own pasta and took a lot of joy in making it. I was also big on takeaways, Indian food, pizzas and burgers and buying food heavy in starches. I didn’t care enough about how I looked or about my diet to change any of my eating habits.
I would happily glug a litre of freshly squeezed juice a day. I’d eat a Mars Bar before a meal, I thought I was invincible when it came to food. I used to travel the world looking for great food and that inevitably contained potatoes, bread, starches and carbs. I veered between fine dining and easy comfort food and takeaways.
TM: Loving food so much, to change things so radically must have been difficult?
RS: When I changed, the reason I decided not to go low-calorie was because I love cooked food, I still do to this day, but I decided to take out of my diet carbs and sugars. That still leaves a whole incredibly rich canvas of food, so I could continue to cook good food.
There are two different parts to this. There’s the period of weight loss where you have to be a little bit ruthless and then when you come out of that, I was fortunate enough to recover enough insulin function to be able to again tolerate some carbohydrates and sugars, so I could resolve a normal diet, but not my former diet, not pasta and pizza, potatoes and rice. So I continue to eat good food to this day and did to an extent when I was on my diet.

TM: So do you stick to low carb now?
RS: Not quite. When I came out of the weight loss I realised low carb wasn’t a long term lifestyle for me. So I experimented with what carbs I could tolerate and I found a good medium for me. So I can eat bread, but I don’t eat it all day. So I’ll have a piece of toast in the morning, but for dinner, I’ll just have proteins, vegetables and fruit.
TM: Where do you stand on proteins?
RS: So, the solution that I came up with was that I was simply going to take out carbs and refined sugars and leave everything else in place, and that included protein and also dairy. So my diet was made up of meats, usually chicken, vegetables, some fruits and full-fat dairy, that was how I achieved the weight loss. And to a large extent that continues today.
TM: How important was keeping a food diary?
RS: I guess I wrote it as therapy to partly understand what I was doing, but by the end because I was pretty sure I’d done it, I decided to be a little more disciplined about it. So I did come up with the book of meals, which became the book as it is.
Although I was recording what I was genuinely eating, I did find the perfect daily meals, and weekly ones and so on and so forth. Nothing in the book isn’t true, I did literally eat those things for the week and I did have those things for breakfast. That final meal is my perfect meal.
And actually that final recipe for a margarita, I woke up a day after drinking an entire jug of margaritas, that was the thing that kicked off my illness, so that’s a homage to me still drinking. If I hadn’t had that blowout which gave me a massive blood sugar spike and very physical symptoms I could have been walking around for weeks or months more with diabetes.
I don’t drink to excess, but alcohol is a part of my diet. It’s one of the things I get asked most, can I drink? Can I drink beer, wine, spirits?
TM: Was that tough for you to cut out?
RS: Well I was a moderate drinker before. I would have blowouts, that’s the truth of it and it was one particular blowout that left me with such a high sugar spike that I had the problem that I had. I never drank beer in any great quantity, that is quite challenging for diabetics, but I did drink wine and spirits and I did want to be able to go out for a meal and have a glass of wine now and then.
I cut that out for eight weeks, firstly for self-discipline, you eat more if you drink more. So it was only fairly short term and now wine and spirits make up a small part of my diet.
TM: Obviously it’s not just diet, it’s really a big lifestyle shift isn’t it?
RS: Yes, this is a wholesale lifestyle change, so of course you diet for a period of time to lose weight, then your diet should also be modified by the time you get out of the other end of it so that it’s something that’s maintainable.
But in addition to what you put in your mouth, I think it’s a good idea to turn up your metabolism. I’m not a gym bunny, I dislike exercise really, but I did force myself as part of this project, which was to walk at least 10k steps a day.
It didn’t change my life, but it helped. But as I became slimmer it helped add a little bit of tone and stamina and made me feel better. I think it has to be a part of the project, so no carbs or refined sugars, a little bit of calorie reduction at the beginning, drink lots of water and do 10k steps per day. How hard is that?
TM: What do you think when the medical system says the condition is non-reversible?
RS: The verdict is out on the lifelong thing, I really don’t believe you have to be on meds forever. At the back end of the weight loss, if you’re able to come off meds, there are some people that are able to control type 2 exclusively through diet, so through a strict eating regime, keep things in check.
Then there are others who are less carb intolerant who can resume a more normal diet. This is to do with the extent of the beta cell recovery in your pancreas. If your pancreas re-starts to a significant degree and the damage isn’t that significant you can acquire greater capacity, you can live on the brink.
There are lots of forums you can read that will say once a diabetic always a diabetic, like being an alcoholic. Actually, if I have perfect blood scores and I can eat pretty much what I want and if I don’t take meds, then I don’t consider myself to be diabetic anymore because the definition of a diabetic means your blood will be above a certain score and your insulin resistance is impaired. This debate is very, very heated in the diabetic community.
I believe the medical profession in general still believes it’s a lifelong chronic, progressive disease and it’s time to change that.
TM: Maybe we can finish with some of your tips for those at risk, or those who might be at that pre-diabetes stage and not realise it…
RS: I think people most at risk are those in their mid-forties to late fifties. If you’re in that age range and are overweight and you find yourself being excessively thirsty, peeing a lot and suddenly losing weight, then those are three classic symptoms. And the way to guard against that, I’m going to be really brutal here, you need to find a way of reducing body fat, that is the real killer. And visible fat is masking the internal visceral fat that is doing all the damage.
So if you fall into that age range and find you have those symptoms happening to you and you have that belly girth, then I think it’s time to think about whether you’re prepared to be diagnosed as type 2 diabetic. The consequences of that there is something you can do about it. This is not an inevitable progressive disease, you can live longer and have a happier family life and all of that.
I guess my five tips are the things I say in the book cut out carbs, cut out refined and processed sugars, restrict your calorie intake for a short period of time, drink plenty of water and get exercise, that’s what it boiled down to for me. The other message I took from the study that came out of Newcastle is the window isn’t open for very long, with pancreatic β-cell recovery the odds shorten a lot after a number of years, so it’s worth giving it a shot.
Conquer Type 2 Diabetes: How a fat, middle-aged man lost 31 kilos and reversed his type 2 diabetes is out to buy now. 
Click the banner to share on Facebook



